The Operating Room Where Doctors Never Washed Their Hands: How Surgery Went From Death Sentence to Day Surgery
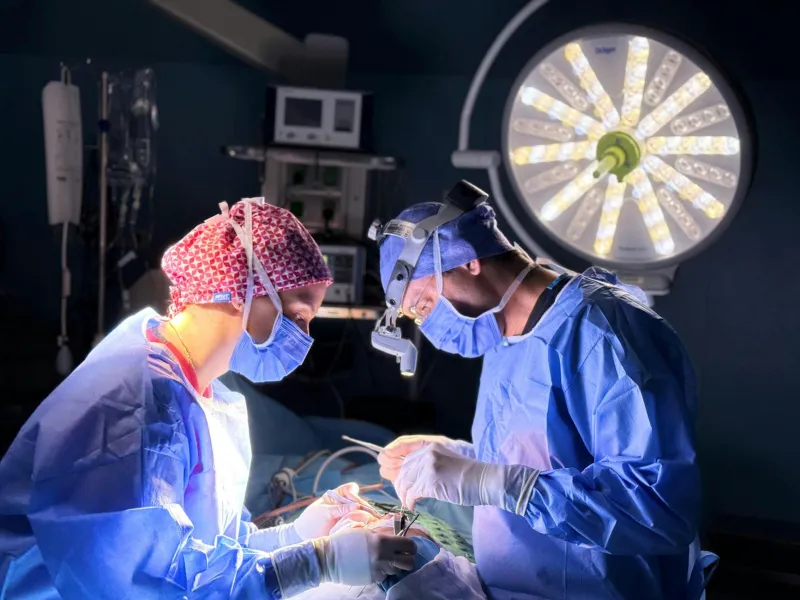
The Blood-Soaked Badge of Honor
Picture this: You're wheeled into an operating room in 1850. The surgeon approaches wearing a coat so stiff with dried blood and pus that it could practically stand up on its own. He's proud of that coat — it's proof of his experience. The more gore caked on the fabric, the more operations he's performed. He doesn't wash his hands because nobody knows germs exist yet, and honestly, why would you wash something that isn't visibly dirty?
This wasn't some back-alley butcher shop. This was state-of-the-art medical care at the finest hospitals in Europe and America.
Today, that same surgeon would be arrested before he made it through the hospital lobby.
When Hospitals Were Deadlier Than Battlefields
The numbers tell a story so shocking it's hard to believe. In the 1840s, if you had surgery in a hospital, you had roughly a 50% chance of dying — not from the operation itself, but from infection afterward. At Vienna General Hospital, the maternity ward run by doctors had a death rate of 18%. The ward run by midwives? Just 2%.
Nobody could figure out why.
Meanwhile, if you got the same surgery at home, your chances improved dramatically. Wealthy patients routinely refused hospital care, preferring to have operations performed on their kitchen tables. They weren't being dramatic — they were making a statistically sound decision.
Compare that to today: The infection rate for most surgeries in American hospitals is well under 3%. You're literally safer having your appendix removed in a modern hospital than you were getting a haircut in some 19th-century barbershops.
The Doctor They Called Crazy
Ignaz Semmelweis was a Hungarian physician working in Vienna when he noticed something odd. The maternity ward staffed by medical students had death rates nearly ten times higher than the one staffed by midwives. The only difference? The medical students spent their mornings dissecting corpses, then went straight to delivering babies without washing their hands.
Semmelweis had a wild theory: What if the medical students were carrying something invisible from the dead bodies to the living patients?
He instituted mandatory hand-washing with chlorinated lime solution. Death rates plummeted overnight — from 18% to less than 2%.
The medical establishment's response? They fired him and blacklisted him from the profession. Colleagues were insulted by the suggestion that gentlemen's hands could be unclean. Semmelweis spent years trying to convince other doctors, failed, and eventually suffered a mental breakdown. He died in an asylum in 1865, ironically from an infection.
The Germ Revolution
It took another twenty years for the medical world to catch up. Louis Pasteur's germ theory finally provided the scientific framework to understand what Semmelweis had observed. Joseph Lister began using carbolic acid as an antiseptic during surgery in the 1860s, and survival rates improved so dramatically that even skeptical colleagues couldn't ignore the results.
But change came slowly. As late as the 1890s, many American surgeons still operated in street clothes, believing that changing into clean surgical attire was an unnecessary European affectation.
From Guesswork to GPS Precision
The transformation didn't stop with hand-washing. In 1900, if you needed surgery, the doctor made his best guess about what was wrong based on your symptoms. X-rays were brand new and considered almost magical. Anesthesia was still primitive — many patients died from the ether itself.
Today, surgeons can see inside your body in real-time with CT scans, MRIs, and ultrasound. They can perform heart surgery through incisions smaller than a keyhole. Robotic systems allow surgeons to operate with precision measured in fractions of millimeters. What used to require weeks of recovery now sends patients home the same day.
The Antibiotic Game Changer
Perhaps nothing transformed medicine more than Alexander Fleming's accidental discovery of penicillin in 1928. Before antibiotics, a simple cut could kill you if it got infected. Pneumonia was called "the captain of the men of death" because it was so reliably fatal.
By the 1950s, diseases that had terrorized humanity for millennia became minor inconveniences. Strep throat went from a potential death sentence to a prescription and three days off work.
The Routine Miracle
Here's what really drives home how much has changed: In 1900, the leading causes of death in America were pneumonia, tuberculosis, and diarrhea. Today, you can get all three treated at an urgent care clinic between your morning coffee and lunch meeting.
We've become so accustomed to medical miracles that we barely notice them. You can have surgery to fix a torn meniscus and be back playing basketball in six weeks. Your grandmother might have limped for the rest of her life with the same injury.
The Price of Progress
Of course, this transformation came with new challenges. Modern healthcare is expensive in ways our ancestors couldn't have imagined. A single CT scan costs more than most people earned in a year in 1900. But here's the thing — that CT scan can diagnose problems that would have been complete mysteries to doctors just a century ago.
The next time you walk into a hospital, remember: You're entering what was once the most dangerous building in any city. Today, it's probably the safest place you could be if something goes wrong with your body. That transformation happened in the span of just a few generations — a blink of an eye in human history, but long enough to completely revolutionize what it means to get sick in America.